Revision Resources
Recent Posts View All
February 2019 FOAMed
Normal Lactate, but a Sick Patient… Lactate is Not Everything
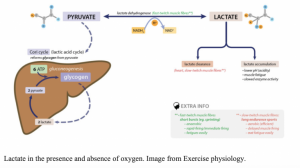
A 57-year-old male with past history of HTN, CAD, and cocaine abuse is brought in by EMS with a fever of 102 °F. Upon questioning, the family mentions decreased PO intake in the last week, decrease urinary output, cough, and several episodes of non-bilious, non-bloody emesis. The cough is productive and worsening. Vital signs upon arrival are 102.5 F, 120 bpm, 23 RR, BP of 120/60, and O2% 95. The patient is conversant but appears toxic. You decide to activate a sepsis code, start your 30 ml/kg IVF bolus, antipyretics, draw labs included in the sepsis protocol, and initiate broad-spectrum antibiotics.
Lab results demonstrate a lactate of 1.5 mmol/L. Clearly something is wrong; that result cannot be real, as the patient appears toxic. You decided to send it again, and this time it returns at 1.4 mmol/L. What could be going on?
Dog Bite Management: The Evidence

I started writing this review of dog bite management a long time ago, but I abandoned it because I thought the word was already out. I thought this had been settled; that everyone knew these myths. However, a few recent conversations have highlighted the fact that the management of dog bites is still steeped in controversy with wide practice variations. Therefore, we will dust off some old papers and see what EBM has to say (and it might be a little more complicated than I remembered)…
Accidental Hypothermia and Cardiac Arrest

A 28-year-old male is found down in a snowbank. He was last seen leaving a nearby bar a few hours prior. The outdoor temperature is -16°C. There is no previous medical history available. Paramedics find him to be pulseless and CPR is initiated immediately. The initial rhythm is ventricular fibrillation (VF). While en route to hospital he is given a total of 4 mg of epinephrine, 450 mg of amiodarone and received 3 defibrillations but remains in VF. EMS is unable to get a temperature peripherally. Upon arrival to hospital the patient’s pupils are 3 mm and sluggish bilaterally. There are no signs of external trauma. A STAT ABG is sent off. Capillary glucose is 10 mmol/L.
Approach to Adult First Time Seizure in the ED

Originally published at CoreEM.net, dedicated to bringing Emergency Providers all things core content Emergency Medicine available to anyone, anywhere, anytime. This is a nice review of first seizure management in the ED.
Le Fort Fractures
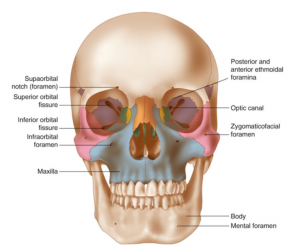
Originally published at CoreEM.net, dedicated to bringing Emergency Providers all things core content Emergency Medicine available to anyone, anywhere, anytime. This review covers the classification, imaging and management of Le Fort fractures.
Are you sure you wish to end this session?

